Examining Global Reproductive Health Funding Cuts and Their Impact
The recent shifts in international donor priorities have sparked major discussions on the current state of reproductive health services worldwide. Over the last decade, many emerging economies made significant progress in reproductive care, with modern contraception reaching record user levels. However, the reduction of international aid—especially by some major donor governments—has left the system feeling both off-putting and tense. In this opinion editorial, we’ll take a closer look at the current scenario, chart the challenges, and figure a path for a more sustainable approach to reproductive health services.
It’s no secret that the efforts invested in reproductive health have a lasting influence on millions of lives. With over 400 million women in low and lower-middle-income countries using modern contraception today, the results speak for themselves. Every call to step up or scale back funding directly translates into unintended pregnancies, unsafe abortions, or even maternal deaths. But what happens when funding sources shift and many programs suddenly find themselves short of money?
Understanding the Shifting Landscape of Reproductive Health Aid
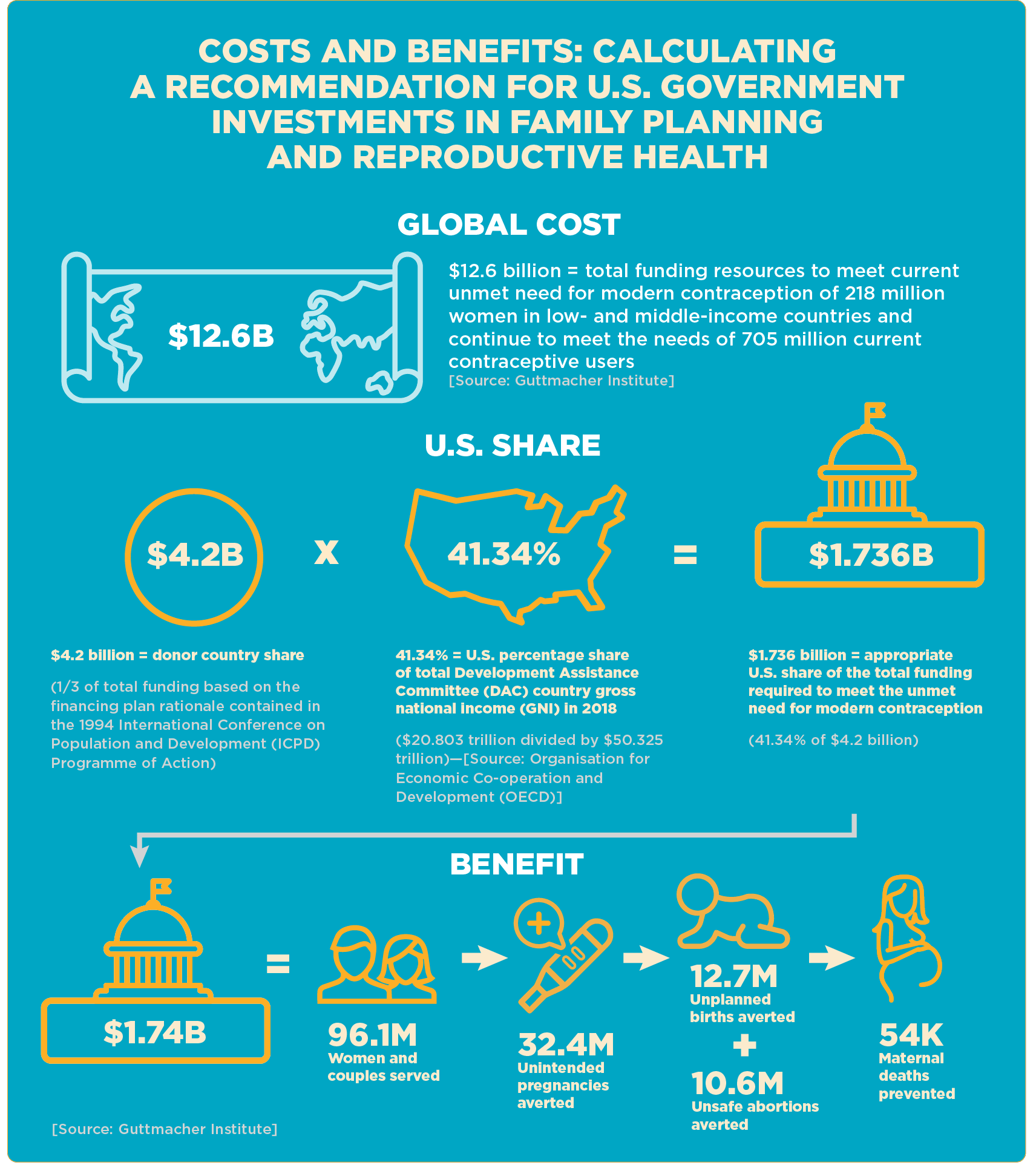
Historically, global reproductive health initiatives received key support from donor governments, with contributions from the United States supplying nearly 41% of the overall financing at one time. With the withdrawal or reduction of funds from major contributors like the U.S., Britain, Germany, and others, many family planning groups are now on the hunt for alternative funding channels.
These funding cuts have led to several ripple effects that have been both intimidating and nerve-racking for organizations worldwide. Experts have pointed out that while many may feel disappointed by the financial constraints, there is an opportunity for nations to think about new sequences and steer through domestic alternatives.
Exploring the Tricky Parts of Donor Withdrawals
When funding pathways become uncertain, organizations are forced to deal with a range of tangled issues. One of the trickiest parts is that donor-dependent health systems become loaded with problems when external money dries up. The unsettling truth is that reliance on foreign aid has sometimes led to expensive oversights, and in many cases, the strings attached to such funds have complicated the nature of service delivery.
Several elements contribute to these tangled issues:
- Reduced funding can directly lead to cuts in essential programs, such as contraceptive distribution and youth health initiatives.
- Staff layoffs and diminished community outreach programs hamper the ability to address local health needs.
- Countries that outsource key aspects of health and education may find themselves scrambling to rebuild those frameworks when donor support falters.
This scenario isn’t just a financial setback—it has a ripple effect on community health outcomes and pushes governments to search for alternative, often local, resources to finance the critical services that women depend on.
Detailing the Hidden Complexities in Global Family Planning Funding
It is essential to take a closer look at the nitty-gritty details behind global family planning investments. Over the last decade, 101 million more people have gained access to modern contraceptives compared to 2012. More importantly, the use of such methods in 2024 is estimated to have averted 148 million unintended pregnancies, 30 million unsafe abortions, and 128,000 maternal deaths worldwide.
These impressive numbers, however, also highlight how delicate the system is. A slip in funding is not merely an economic blip—it represents a sharp downturn in the capacity to save lives. The table below outlines some of the key investment points and impacts over the past years:
| Key Metrics | 2012 | 2024 (Estimated Impact) |
|---|---|---|
| Increase in Contraceptive Access | Baseline | +101 million people |
| Averted Unintended Pregnancies | N/A | 148 million |
| Averted Unsafe Abortions | N/A | 30 million |
| Averted Maternal Deaths | N/A | 128,000 |
From these figures, it is clear that the benefits of sustained investment in reproductive health are super important. The challenge now for policymakers and advocates is to safeguard these gains and counterbalance the financial void left by donor withdrawals.
Identifying Domestic Alternatives: Paving a New Way Forward
In light of shrinking international funds, many local governments and non-governmental organizations are beginning to get into the discussion on how to ensure continuous financing. While the shift from foreign aid to domestic funding may seem overwhelming at first, it can also lead to a more autonomous and sustainable system.
Here are a few strategies that local bodies and governments might consider:
- Reprioritizing National Budgets: By reallocating domestic funds towards healthcare, governments can ensure constant support for critical services.
- Engaging Local Philanthropy: Local businesses and philanthropic entities can work together to bridge the funding gap, contributing resources where they are needed most.
- Encouraging Private Sector Partnerships: Collaborations with private health companies can provide both innovation and investments into reproductive health projects.
- Community-Based Funding Initiatives: In some regions, community funding programs have emerged, pooling local resources to provide for essential health services.
Each of these strategies represents a way to make your way through a funding landscape that has been riddled with sudden twists and turns. Instead of waiting anxiously for international guarantees, many experts now argue that local innovation and self-sufficiency are the best route to take for building resilient health care systems.
Financial Challenges: The Small Distinctions in Cost versus Investment
Beyond the immediate issues of donor dependency, there is also an important conversation centered around the cost of providing comprehensive reproductive health services. According to recent reports, nearly $104 billion is needed annually in low and middle-income nations to meet all sexual and reproductive health needs. That number, while massive, translates into an extra cost of just $8.05 per recipient—a price that many compare to the cost of a cappuccino in wealthier countries.
Given that each dollar invested in contraceptive services can save an estimated $2.48 in maternal, newborn, and abortion care costs, the argument in favor of additional funding becomes even more critical. The fine points of these calculations underscore the economic benefits that go beyond immediately measurable health metrics. They help make the case for why boosting investment in reproductive health isn’t just a moral imperative—it’s a smart economic policy.
Learning from the Past: Historical Lessons and Modern Implications
The history of global family planning is full of lessons that show the scary realities of withdrawing support too quickly. For instance, in Malawi, drastic cuts in U.S.-based funding resulted in a layoff of roughly 4,000 health professionals, effectively removing nearly half of the country’s total health workforce from reproductive care programs.
This scenario is not unique to Malawi. Across many countries, sudden cuts have left health programs struggling to maintain progress. Several commentators have stressed that by outsourcing critical elements of healthcare to foreign donors, many nations inadvertently made themselves vulnerable to shifts in global politics and donor priorities.
Critics have argued that this dependency on external funding has often led to not only financial instability but also a loss of local control over healthcare priorities. As nations now attempt to regain control, there is a growing push toward establishing systems that are less reliant on international sources. These national initiatives, whether they involve increased government funding, localized health insurance schemes, or community health projects, could help secure a more stable future.
Managing Your Way Through Risk: The Psychological Impact on Health Workers
It’s important to recognize that funding instability affects not just patients but also the countless health workers who are tasked with delivering frontline services. The uncertainty brought about by donor withdrawals is often described as overwhelming and nerve-racking by those working on the ground. When funding is unpredictable, job security is compromised and many skilled professionals feel forced to either cut corners or leave the field entirely.
For instance, providers have to figure a path through the reduced availability of basic supplies, training opportunities, and even adequate compensation. These distracted working conditions can ultimately impact the quality of care available to women and girls needing consistent reproductive health services.
Here are some of the key challenges faced by health workers as a result of funding cuts:
- Reduced Staffing Levels: Layoffs and slower hiring rates lead to increased workloads and longer wait times for patients.
- Limited Access to Training: Without sufficient funds, continuing education and professional development become off-putting, resulting in potential skill gaps.
- Scarcity of Medical Supplies: Budget cuts may force facilities to make do with fewer medicines and equipment, directly impacting service quality.
Many in the healthcare field are calling for more secure and locally controlled funding alternatives that can ensure a steadier flow of resources, ultimately allowing health workers to focus on what they do best: providing quality care without the worry of financial instability.
Shifting Political Winds: The Influence of International Policies
The broader picture of reproductive health funding is complicated by geopolitical factors. International politics play a significant role in determining which areas receive funding and which do not. The recent disputes over funding priorities have highlighted how international trends directly influence local outcomes. For example, cuts in USAID budgets have had a pronounced impact on youth health programs in regions like the Asia-Pacific—areas that already have a significant number of reproductive-age women.
Political decisions at the highest levels can cause subtle shifts or even dramatic swings in the support system available to developing nations. These political winds not only influence which projects get funded but also affect public opinion and local government agendas. In many cases, the decisions taken by donor countries have left small nations forced to manage the sudden gap in support—often with mixed results.
This situation calls for global cooperation and the rethinking of aid models. Instead of over-relying on a handful of wealthy nations that may alter their contributions with changing political climates, a more diversified and locally grounded funding strategy might help ease the tension. Such a strategy requires that all stakeholders, including governments, non-profits, and private enterprises, join forces to build a stable foundation for reproductive health services.
Charting the Future: Rethinking the Global Health Architectures
The need for reform in global reproductive health financing cannot be understated. Experts across the board agree that it’s time to take a deeper look at how health systems are built and funded on a global scale. Rather than sticking to the same old formulas where donor money flows in regularly, stakeholders must work through both the tricky parts and the more subtle distinctions to develop an innovative approach to funding.
There are several key elements that must be part of this new architecture:
- Shared Responsibility: There should be a balanced contribution from national governments, donor agencies, philanthropic organizations, and the private sector.
- Sustainable Funding Models: Moving away from donor dependency toward self-sustaining models ensures that health services are preserved even when international support is volatile.
- Local Empowerment: Enhancing local control and involving community leaders in decision-making can help tailor services to better meet specific needs.
- Transparent Governance: Accountability and openness in how funds are managed are critical to rebuild the confidence that has been lost due to cuts and inconsistencies.
Reforming the global health architecture requires everyone to get into the discussion. Policymakers are now being urged to take the wheel and figure a path that paves the way for enhanced domestic investments. The process calls for rethinking budget priorities and reviewing how strategic funding can be channeled into life-saving programs that save not only money but also lives.
Mobilizing Community Support: The Role of Grassroots Movements
As international funding diminishes, grassroots movements and local community initiatives gain even more significance. These community-based projects often act as the final safety net for women who depend heavily on reproductive health services. Grassroots organizations have a unique advantage—they understand the local context and are able to bridge the gap between policy and practice.
Community mobilization in recent years has taken several innovative forms:
- Local Fundraising Campaigns: Small-scale campaigns have shown impressive results in raising awareness and financial support for local health projects.
- Volunteer Networks: Communities have pooled volunteer efforts to maintain community health centers and provide necessary education on family planning.
- Partnerships with Social Enterprises: Emerging social enterprises in the healthcare sector offer innovative solutions and have often contributed essential funds during times of crisis.
The subtle details of these community efforts—although they may appear as small distinctions—play a critical role in reinforcing the overall system. They not only provide the much-needed services on the ground but also serve as a model for self-reliance and cooperation, demonstrating that even when international aid falls short, communities can work together to fill the gap.
Comparing International Models: Insights from Different Regions
Looking at how different regions are managing their reproductive health funding can offer valuable insights. Countries in Africa, Asia, and Latin America have each adopted unique approaches to managing the fallout from reduced international aid.
Consider the following bullet points summarizing key strategies:
- African Nations: Many African countries are increasingly investing in national health insurance schemes and collaborating with local non-profits to offset foreign aid declines.
- Asian Strategies: In parts of Asia, such as India and Nepal, local NGOs have stepped in to provide subsidized contraceptives and community education in response to major donor cuts.
- Latin American Efforts: In some Latin American nations, governments have reallocated national budgets to protect key family planning programs, ensuring continuity despite reduced external funds.
Each of these approaches offers a glimpse into how local context matters. While all regions face tense challenges due to external pressures, the way they manage to sort out these issues depends on the fine shades of local politics and economic landscapes. The lessons learned from these diverse models can be adapted and applied in other regions facing similar difficulties.
Policy Recommendations: A Call for Equal Responsibility
Given the full spectrum of challenges and the effects of international funding shifts, it is clear that a collective effort is needed to ensure reproductive health advances aren’t stalled. Policymakers and international leaders must work together to create an environment where shared responsibility becomes a guiding principle.
Below is a summary of critical recommendations that could help in the reformation process:
- Establish Multi-Stakeholder Funds: Create funding mechanisms where governments, private donors, nonprofit organizations, and local communities contribute jointly.
- Encourage Innovation in Funding Models: Leverage technology and social media to mobilize local resources and improve transparency in fund allocation.
- Strengthen Local Governance: Empower local health agencies with both the responsibility and the resources needed to manage reproductive health programs effectively.
- Implement Accountability Measures: Develop systems for thorough auditing and public reporting to rebuild trust among stakeholders.
These recommendations may seem like just a few bullet points, but they capture the little twists and turns that, when addressed, can lead to a stronger and more resilient reproductive health infrastructure.
Conclusion: Rebuilding Confidence in Reproductive Health Funding
The ongoing funding cuts in reproductive health services leave behind a challenging landscape full of twists and turns as well as confusing bits that need to be understood and addressed. While the withdrawal of international funds has indeed startled many, it has also ignited an essential dialogue on how to rebuild a system that can operate even amid financial uncertainty.
We must acknowledge that the progress made over the past decade—marked by record usage of modern contraception around the world—faces a risky setback if donor cuts persist. However, by taking a closer look at the problems, engaging in meaningful community mobilization, and shifting toward more local, sustainable funding models, there is hope for a future where reproductive health services remain accessible and effective.
Ultimately, the path forward is one that calls on shared responsibility and innovative thinking. The stakes are not just economic but deeply human: every unintended pregnancy averted, every unsafe abortion prevented, and every maternal life saved underscores the super important need to rethink and rebuild global reproductive health architectures. By learning from past mistakes and stepping up to the challenges of today, governments, health workers, and communities can work together to secure a future that remains bright even when international funding falters.
As we move forward, it will be key for policymakers, non-profits, and private enterprises alike to work through the tricky parts and navigate the tangled issues faced by health systems worldwide. By taking charge of our funding methods and embracing local, sustainable solutions, we not only protect the progress that has already been made but also lay the foundation for a future where reproductive health is consistently and equitably treated as a public good.
In the end, the debate is not simply about money—it is about human lives, the empowerment of communities, and ensuring that progress never comes to a halt. Let’s commit to working together, sharing responsibility equally, and continually processing the small distinctions that make up the overall mosaic of reproductive health services around the world.
Final Thoughts and a Look Ahead
Looking ahead, it’s clear that the journey to rebuild confidence in reproductive health funding is both challenging and necessary. It calls for rethinking established policies as well as bold innovations in funding strategies. The conversation should no longer be defined by a dichotomy between donor dollars and domestic contributions but rather by a holistic approach that integrates multiple funding channels into one coherent strategy.
We must all get into the conversation and contribute our ideas, whether through local community initiatives or global policy reforms. Only by working together and using every available resource can we figure out a path that secures reproductive health services for generations to come. In doing so, we not only protect lives but also ensure that progress in global health does not follow a downward spiral when keys funds are shifted.
This perspective offers a roadmap for creating a more inclusive, resilient, and self-sustaining reproductive health ecosystem where every woman, regardless of her location or socioeconomic status, can access the care she needs. It is our collective responsibility to stare down these challenging times, find our way through the maze, and build a future that stands as a testament to the power of collaborative, community-focused action.
Originally Post From https://bilyonaryo.com/2025/11/08/experts-warn-funding-cuts-risk-setbacks-in-reproductive-health/health/
Read more about this topic at
The Ripple Effects of the US Retreat from International …
The Trump Administration Is Endangering Women’s …


